ICU patients often suffer from compromised immune systems due to their underlying medical conditions, invasive procedures, and the use of immunosuppressive medications. This weakened defense system leaves them highly susceptible to infections, which can significantly impact their recovery and overall health. Hospital-acquired infections (HAIs), also known as healthcare-associated infections, are quite common in in ICU patients. These infections can increase hospital stay and associated cost- some studies show HAIs can increase stay by an average of 8.3 days.
Many of these infections are the result of contact with contaminated stool, as feces contain a number of infectious pathogens. ICU nurses frequently utilize a closed fecal management systems or devices (FMS or FMDs) to divert fecal matter away from patients, thereby protecting both the patients and their immediate surroundings from potential contamination. This approach helps mitigate the risk of infection transmission significantly.
Cross-contamination with fecal pathogens is a serious consideration. Fecal-oral transmission can spread many common infections, such as E. coli, hepatitis A, campylobacter, adenovirus, giardia, Salmonella, and Shigella, and each can lead to compromised patient health and extended length of stay. C. difficile (C. diff) infection is especially common and problematic. Transmitted via the fecal-oral route, C. difficile infection (CDI) is the most common cause of diarrhea in the ICU. CDI develops as the result of the normal bacterial flora of the colon, colonization by C. diff, and toxin release that cause mucosal damage and inflammation. The concerning aspect is that C. diff bacteria can disseminate through the feces of infected individuals, and healthcare personnel, as well as others, can inadvertently transfer these contaminated feces to various surfaces. This cross-contamination can occur within the patient’s individual ward and extend throughout the hospital. C. diff spores can survive on inanimate surfaces for up to 5 months, and are resistant to most disinfectants and decontamination techniques used in hospitals.
The prevalence of infection in ICU is about 0.4%-4% and has severe effect on morbidity and mortality rates. The hospital mortality rate of CDI patients is approximately 10.2-32% and the rate of first recurrence is estimated to be 13.5% in patients with community onset colitis C.difficle infection. The HAI leads to an additional LOS of 2.9-11.1 days and additional cost of about $7286-$29000. Additionally, approximately 10%-20% of patients are colonized from the infections without indicating any symptoms of it.
Clearly, infection control measures are essential for preventing complications and improving patient outcomes.
Cross-contamination from Fecal Incontinence in ICU Patients
Like other units in hospital settings, ICUs have largely relied on absorbent pad and intrarectal balloon catheters (IBCs) to manage fecal incontinence, but these FMDs may be inefficient to isolate microorganisms from the patients’ surroundings. Absorbent pads do not adequately contain fecal effluents, which can create a robust biome for microorganisms. In order to contain fecal effluents efficiently, a closed system is required that does not leak. Several reports have been observed on FDA MAUDE database for IBCs and associated frequent leakage, which can lead to complications such as skin necrosis and Incontinence-Associated Dermatitis (IAD).
Nearly every step of FMD use presents the potential for contamination, and therefore, infection. Even the shape of the FMD or the removal of the device can pose the risk of infection. A 2019 study published in Wound Management & Prevention showed that the design of the FMD device influences the contamination and potential risk of infection.
Qoramatic – first ever automated Stool Management Kit that can help improve clinical outcomes while also reduce nursing burden!
Fortunately, advances in technology can help free patients (and nursing staff) from the burden of HAIs, and especially those associated with fecal management devices. A closed fecal management system can help prevent the spread of infectious spores by isolating the infected individual’s feces, reducing the risk of cross-contamination to other patients and healthcare workers.
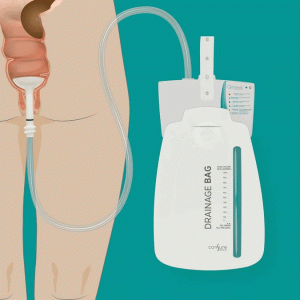
It has a soft silicon indwelling receptacle that exerts zero radial pressure on rectal mucosa significantly minimizing incidences of necrosis, rectal bleeding, sphincter injury. Unlike high pressure balloon catheters, the receptacle does not require any inflation, eliminating the incidences of medical errors around over inflations and complications associated with it. The system has inbuilt suction and irrigation chamber which reduces manual interventions and saves up to 174 minutes of nursing time.
To learn more about Qoramatic or to get a free demo, contact [email protected].