Gallbladder disease is a relatively common condition, affecting about 20.5 million people in the U.S. Cholecystectomy, the surgical removal of the gallbladder, is a standard procedure performed worldwide, with over 700,000 surgeries each year. Despite the surgery being recognized as safe and effective, but it is crucial to understand its potential side effects, including fecal incontinence. According to the latest research findings, approximately 9 percent of individuals are affected by fecal incontinence after surgery.
Understanding Cholecystectomy and the Gallbladder
The gallbladder is a small, pear-shaped organ located under the liver. Its primary function is to act as a reservoir for bile, a digestive acid the liver produces. Bile aids in the digestion and absorption of fats in the small intestine. Cholecystectomy is commonly performed when complications such as gallstones, pancreas inflammation, or other gallbladder-related issues occur.
The Relationship Between Cholecystectomy and Fecal Incontinence
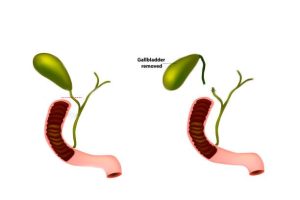
Gallbladder: A reservoir for Bile; Image Credits: Chanu Dasari MD
While cholecystectomy is generally considered safe, it can lead to various postoperative symptoms, including fecal incontinence. Fecal incontinence refers to the inability to control bowel movements, resulting in unintentional leakage of stool.
In the case of cholecystectomy, the higher concentration of bile in the small intestine resulting from the absence of the bile-storing organ can result in persistent diarrhea. While the anal sphincter muscle can effectively retain solid waste, there is a possibility of leakage of watery or liquid stool through the anus. Consequently, individuals may experience sudden urges to use the restroom or may struggle to control bowel movements until reaching a toilet. Recent studies have found that this can occur in up to 17 percent of people after gallbladder removal. Men younger than age 50, especially if they are obese, have the highest likelihood of long-term diarrhea after gallbladder surgery, but a significant number of people without those risk factors may also have intermittent diarrhea for months to years after surgery.
Diagnosis and Treatment of Fecal Incontinence
Statistics indicate that individuals experiencing fecal incontinence may feel embarrassed or hesitant to seek treatment. However, it is crucial to emphasize that managing incontinence is necessary to enhance quality of life. With proper diagnosis and treatment, most people can successfully manage their fecal incontinence and regain control over their bowel movements, enabling them to live an everyday life.
To effectively manage fecal incontinence post-cholecystectomy, a comprehensive approach is necessary. Healthcare providers play a vital role in diagnosing the condition and implementing appropriate treatment strategies. The diagnostic process may involve:
- A thorough medical history review.
- Physical examination.
- Additional tests to identify any underlying causes contributing to fecal incontinence.
Treatment options for fecal incontinence can include lifestyle modifications, such as dietary changes to regulate bowel movements and incorporating pelvic floor exercises to improve muscle control. Medications, such as antidiarrheal agents or bulking agents, may be prescribed to alleviate symptoms.
Strategies for Coping with Post Cholecystectomy
Understanding the different mechanisms and adjusting after gallbladder removal is crucial for adapting to a new way of life. While these changes may initially feel uncomfortable, they become more manageable over time.
Limit Fat Intake: Since gallbladder removal can reduce the effectiveness of bile, it is important to moderate fat consumption. This involves opting for healthier cooking methods such as steaming, baking, boiling, or grilling, while avoiding fried foods that are high in fats.
Lifestyle Adjustments: Long-term comfort can be enhanced by adjusting your lifestyle and activities. Being aware of your condition and mindful of your actions is key. This includes being mindful of the types of exercises you engage in, paying attention to your diet and the timing of meals to prevent issues like bloating.
While cholecystectomy is a commonly performed surgical procedure for various gallbladder-related issues, it is essential to be aware of potential complications, including the development of fecal incontinence. Increased bile delivery to the small intestine post-cholecystectomy can contribute to bowel leakage and incontinence in some patients. Breaking the stigma surrounding incontinence is crucial, encouraging individuals to seek proper diagnosis and treatment. With the guidance of healthcare providers and comprehensive management approaches, most people can effectively manage fecal incontinence and lead fulfilling lives.

One reply on “Is Cholecystectomy Responsible for Causing Incontinence?”
Blue Techker I very delighted to find this internet site on bing, just what I was searching for as well saved to fav