Colitis C.difficle or Clostridium difficile results from a disturbance of the normal bacterial flora of the colon, colonization by C difficile, and the release of toxins that cause mucosal inflammation and damage. The bacteria spreads through feces of infected individual and can survive on surfaces for a long duration. They typically infect people which are recently treated with antibiotic, as drugs can disrupt the normal balance of bacteria in the gut which allows C.difficile to grow unchecked. The bacteria can give rise to inflammation in the colon leading to various symptoms such as fecal incontinence, abdominal pain and fever.
Colitis C.difficle infection is one of the leading causes of healthcare associated infections and is common in hospital settings. It is estimated that CDI causes 500,000 infections and 29,000 deaths in a year. Over the past years, there is a significant increase in the cases and severity of Clostridium difficile infection in critical care unit. The prevalence of infection in ICU is about 0.4%-4% and has severe effect on morbidity and mortality rates. The hospital mortality rate of CDI patients is approximately 10.2-32% and the rate of first recurrence is estimated to be 13.5% in patients with community onset colitis C.difficle infection. The HAI leads to an additional LOS of 2.9-11.1 days and additional cost of about $7286-$29000. Additionally, approximately 10%-20% of patients are colonized from the infections without indicating any symptoms of it.
As mentioned above, in severe cases CDI causes fecal incontinence, the inability to control bowel movements resulting in an involuntary passage of feces. This may occur due to inflammation which can damage the muscles and the nerves in the colon that control bowel movements, making it difficult to hold fecal exudate. This can have a significant impact on an individual’s quality of life, clinical outcomes and hospital quality metrics. Below are some basic principles and intervention recommendations for the prevention and containment of Clostridioides.
Ways of managing Colitis C. difficile

Image Courtesy: DC Studio, Freepik
Diagnosis:
The first step in managing CDI is to accurately diagnose the infection. Cell cytotoxicity test is a stool culture laboratory testing method to detect presence of C.difficile toxins. stool samples are done to detect the presence of C difficile toxins. It is important to note that not all patients with diarrhea will test positive for CDI, as other causes of diarrhea such as norovirus or Clostridium perfringens can also cause similar symptoms. Therefore, it is important to consider other possible causes of diarrhea when interpreting test results.
Isolation:
Patients with CDI should be placed in isolation to prevent the spread of the infection to other patients in the ICU. This can be done by placing patients in a private room or by using contact isolation precautions, which include the use of gowns, gloves, and masks when caring for the patient. It is also important to ensure that any equipment or surfaces that come into contact with the patient’s feces are properly cleaned and disinfected to prevent the spread of the infection.
Hygiene:
Hand hygiene is one of the most important measures for preventing the spread of infection. Healthcare workers should wash their hands
frequently and thoroughly, especially before and after caring for patients.
Use of Personal Protective Equipment:

Image Courtesy : Advent Health University
Personal protective equipment (PPE) such as gowns, gloves, and masks should be used. This is particularly important when cleaning the patient’s room or handling their feces. Gowns and gloves should be changed after each encounter with the patient and should be disposed of properly.
Antibiotic Stewardship:
Antibiotic stewardship is an important aspect of managing CDI in the ICU. Antibiotics are a major risk factor for the development of infection as they disrupt the normal gut flora and allow C difficile to proliferate. Therefore, it is important to use antibiotics judiciously and to choose antibiotics that are less likely to disrupt the gut microbiome. Additionally, patients should be treated with specific antibiotics, such as metronidazole or vancomycin, to eliminate the C difficile infection.
Environmental Cleaning:
Proper environmental cleaning is crucial in preventing the spread of CDI. All surfaces in the patient’s room should be cleaned and disinfected regularly, using a bleach-based solution. Special attention should be paid to high-touch surfaces such as toilets, bedside tables, and door knobs.
Closed Fecal Management System:
A closed fecal management system can help prevent the spread of C. difficile spores by isolating the infected individual’s feces, reducing the risk of cross-contamination to other patients and healthcare workers It is important to utilize an appropriate management option to improve their symptoms and reduce any negative effects on their life.
Qora Stool Management Kit
Qora is the first non-balloon closed stool management system (also referred to as fecal bags) which voids the rectum and diverts stool away from the patient in an external collection bag. The device is designed to be comfortable and easy to use, which can help to improve the overall experience for patients dealing with CDI. Certain features of Qora SMK add additional benefits for care providers and patients with CDI.
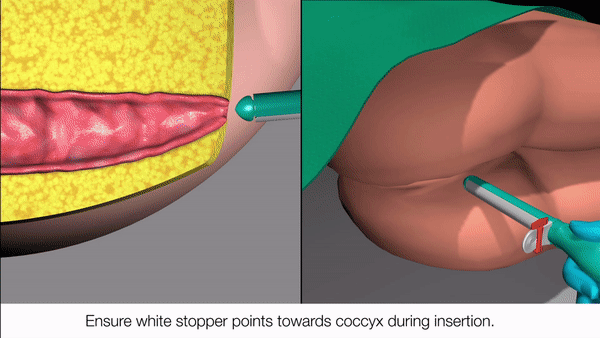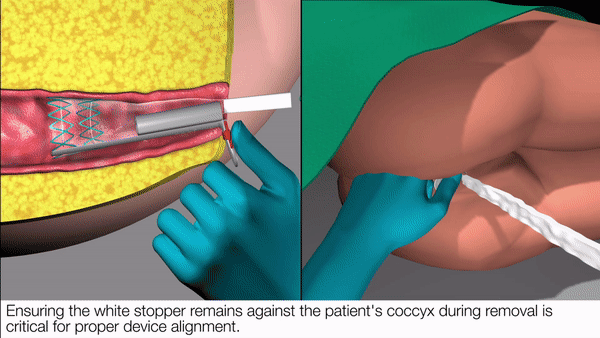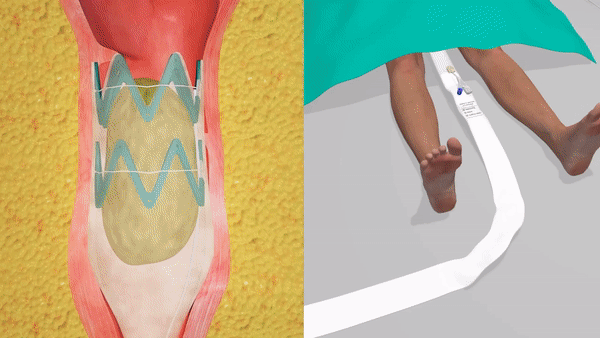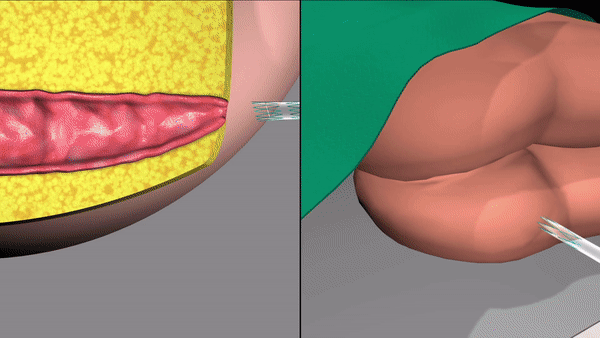
Qora’s novel self-expanding lattice
Ergonomic applicator insertion mechanism instead of digital insertion ensures hygienic and accurate deployment every single time.
Regular testing and diagnosis are an integral part of C Diff patient care strategy. The device employs a stool sampling port that helps in contactless stool sampling using a slip tip syringe. This assists healthcare providers to monitor the patient’s response to treatment and determine when the infection has been eliminated.
The device also allows 2X faster fluid delivery than a balloon catheter for rectal administration of essential medications.
Overall, closed fecal management systems like QORA can play an important role in reducing the spread of CDI and decreasing the risk of recurrence. Qora fecal management system helps keep patients, healthcare providers and the surrounding environment safe while also providing a convenient and effective method of managing fecal waste in patients with Fecal Incontinence.


One reply on “Effective Strategies for Managing Colitis C.diff in ICU”
Packachange I appreciate you sharing this blog post. Thanks Again. Cool.